By Elizabeth Wulfhorst
RED BANK – It’s always difficult when someone in your family gets sick, and when that family member can’t tell you how or when they hurt, it can make diagnosing the problem daunting. When the diagnosis is cancer, early detection is key to effective treatment and potential recovery.
According to the American Veterinary Medical Association (AVMA), “Approximately 1 in 4 dogs will develop cancer at some point during their life.” The risk doubles in older dogs. Cancer can also be a risk for cats and other species, particularly as they age.
But “pets today have a better chance of being successfully treated for cancer than ever before, thanks to major advances in early recognition, diagnosis, and treatment,” the AVMA says.
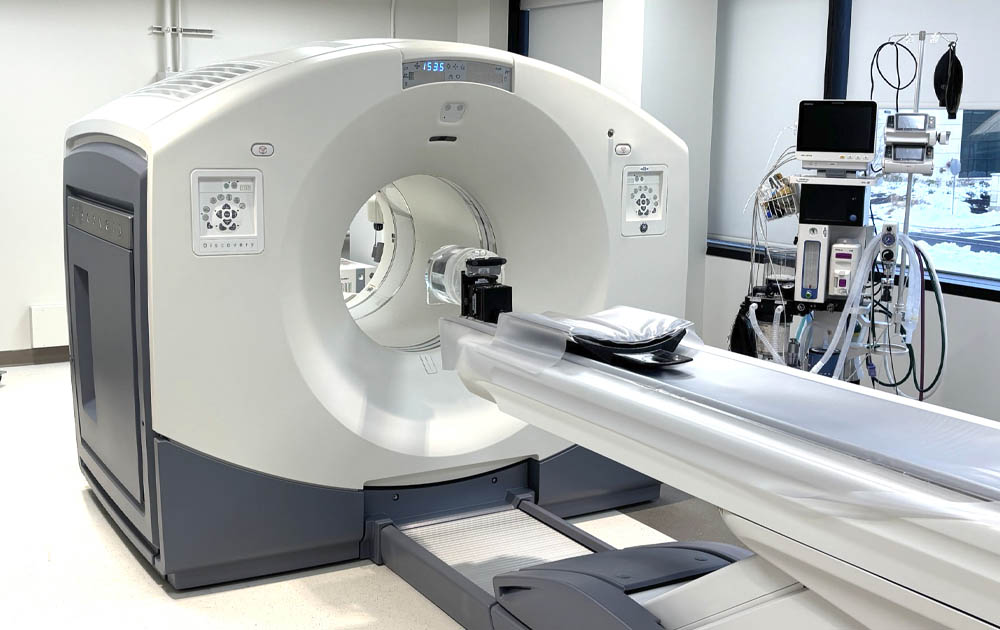
At its not-quite two-year-old facility on Schultz Road near the Garden State Parkway, Red Bank Veterinary Hospital is making that successful treatment happen with medical technology you’d expect to find in a human hospital: positron emission tomography and computed tomography, also known as PET and CT scanning.
This advanced medical technology is only available at a few veterinary hospitals in the country, mostly those associated with veterinary schools and teaching hospitals; RBVH has just the sixth veterinary PET/CT scanner in the country, the only one in a private practice, and the only one east of Ohio.
“As we were designing this building and thinking about what it could and should be and be able to do, we identified PET/CT as a cutting-edge opportunity and something that we can offer that not everyone can,” explained David Conway, D.V.M., associate medical director of RBVH.
“It’s been used for some years, mostly in research, but the clinical applications of it are growing and growing,” he said. The hope is the machine will help improve doctors’ ability to detect and treat disease in pets throughout the region.
“Offering PET/CT at RBVH places us among a very select group of veterinary hospitals nationwide,” said Peter Chapman, BVetMed, DECVIM-CA, DACVIM, MRCVS, the hospital’s medical director, in an earlier release. “This technology empowers our team to diagnose cancer earlier, tailor treatment plans more precisely, and ultimately improve outcomes for our patients.”
Detecting Cancer
The PET/CT machine is exactly the same one you’ll find in a human hospital. The only difference is in how the patient is immobilized during the test. While humans can obey when told to lie still, animals can’t. “In the veterinary case, they’re sedated or anesthetized because they cannot move, or the test is blurry,” Conway said.
The animal patient is placed on the table, which slides in and out of a ring that contains an X-ray detector that spins around hundreds of times, taking thousands of images, Conway explained. “Because it’s doing it so rapidly and in a circle, we get three-dimensional imaging of the patient.”
If a PET scan is required, the animal is injected with a radioactive sugar “that is taken up by tissues throughout the body” during metabolic activity.
“The PET scanner detects those radiant radioactive signatures and then makes these really pretty images with these grayish black blobs of activity,” Conway said. “And if you just have them by themselves, they’re not that useful because you can’t tell what part of the body they’re on. But we use a computer algorithm to stack that on top of our three-dimensional CT scan, and then we can tell what tissues, what structures, have taken up that radioactive sugar.”
While the CT shows the animal’s anatomy, the PET allows doctors to see the function of the tissues.
Some tissues, like the brain and heart, use a lot of sugar, so they will always be bright, “but some tissues, the skin or the bones, really shouldn’t be that bright, unless something’s wrong.”
“Inflammation or cancer is going to cause a rapid increase in the metabolic rate of those tissues as they divide out of control. So we’re looking for those disease processes abnormally using more sugar than they’re supposed to be to find problems,” he said.
Conway calls the machine “the Cadillac of detecting and monitoring many, many types of cancer.” While it is not intended to diagnose every cancer – “we have better tests for some cancers, like brain tumors and pancreatic tumors,” he said – it is far better than diagnostic tools of the past.
RBVH treats a variety of animal species and most of them can benefit from the CT scanner, if warranted. But PET scans can be difficult for smaller animals.
It “is a little more challenging because it requires a longer anesthesia,” Conway said.
“Those really tiny patients are difficult to do that with the safety that we demand, but from a physiology perspective, there’s nothing saying that we can’t.”
Conway has been discussing with the hospital’s exotic service the possibility of launching research in the coming years to break ground in that area, another benefit of having the PET/CT machine.
“We do research here every month, whether that’s a planned project or we see an interesting case and publish it for the benefit of the community,” he said.
A Treatment Plan
While there is “no evidence for an actual rise in the rate of cancer” in pets, Conway said, “certain cancers are becoming more or less common, mostly seemingly with genetics and breeding.”
“But what is changing is that pets are living longer because they’re getting better care, better food, staying inside instead of being out on the farm and being hit by cars. And then as pets live longer, they have more time to develop that cancer, and simultaneously, we have gotten better at detecting and treating it, and clients and owners of pets have gotten more interested in having that diagnosed and treated.”
It can be especially difficult to diagnose early-stage cancer in pets.
“Many pets are good at hiding signs of illness; the signs they show can be subtle or mimic other diseases; and sometimes there simply are no signs until the cancer has reached an advanced stage,” according to the AVMA.
“There’s a huge variety (of symptoms), which is really frustrating for owners, because it depends on which body system is affected with which type of cancer,” Conway said.
Some general signs to look for include loss of appetite and/or unexplained weight loss; abdominal swelling or bloating; difficulty eating, swallowing or breathing; lumps or bumps that grow or change color or texture over time; persistent sores or wounds that won’t heal; and behavior changes, among others.
Conway said there are three “mainstays” of cancer treatment, similar again to the treatments for humans, including surgery, chemotherapy or radiation therapy.
“A lot of the things that we do come from human medicine, because the research dollars for people, as you’d expect, are much greater than what we have. So they will develop something, prove its efficacy,” and then the veterinary field can potentially adopt it.
“As things become generic or become potentially affordable for a normal person to do for their dog or cat, we try to test them and adopt them in a systematic way,” Conway said.
The article originally appeared in the April 9 – 15, 2026 print edition of The Two River Times.














