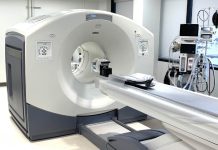
The health care community has redefined the requirements for clinical obesity, noting BMI shouldn’t be the sole barometer of the disease.
By Regina Molaro
Many people dread going to their doctor because they hope to avoid discussing weight gain and obesity and their impact on health. According to the World Health Organization (WHO), obesity is defined as “excess or abnormal fat and accumulation that presents a risk to health.” A chronic disease, obesity affects 4 in 10 adults in the United States.
Obesity is determined by Body Mass Index, or BMI, a numeric value derived from a person’s weight and height. The National Institutes of Health (NIH) cites the origins of this concept as 1832, when statistician Adolphe Quetelet introduced it. In 1972, physiologist Ancel Keys expanded upon Quetelet’s work and coined the term “BMI.”
The BMI-based classifications, which were adopted in the 1990s by the NIH and WHO, were updated last month. Many health experts agree that the previous guidelines were too simplistic.
“Although BMI is easy to measure, it may overestimate the degree of fatty tissue in people that are considered overweight yet muscular (bodybuilders) and underestimate in older people due to muscle mass loss and height from osteoporosis (a bone disease),” said Fatima Asghar, M.D., an internal medicine physician who is board certified in hepatology and is part of the RWJBarnabas Health Medical Group.
Obesity is a complex disease. There is no “one size fits all” approach to effective management. It requires individualized strategies that address specific contributing factors for each person.
A New Direction
The updated guidelines propose a shift from solely using BMI to diagnose obesity to including a waist circumference measurement (Body Roundness Index or BRI). For men, greater than or equal to 40 is considered elevated and indicative of increased cardiometabolic risks. For women, that number is 35.
“Many medical organizations wanted to redefine clinical obesity since BMI alone doesn’t encompass all patients affected by the disease,” said Richard Greco, D.O., Hackensack Meridian Health Bayshore Medical Center in Holmdel. “Patients who are taller have lower BMIs and, despite having signs of organ dysfunction, might not qualify for treatment. The recommendation is to measure excess body fat and how it affects health.”
By adding a waist circumference measurement, adults at increased risk for morbidity and mortality from heart disease, hypertension, diabetes, dyslipidemia and steatotic liver disease can be more accurately identified,” said Asghar. Other comorbidities (the simultaneous presence of two or more diseases or medical conditions) include symptomatic osteoarthritis (especially of the knees), cholelithiasis, depression, obstructive sleep apnea and impaired quality of life.
“The old guidelines for surgical eligibility were strictly based on BMI. That was a BMI of 40, or 35 with at least one medical comorbidity associated with obesity,” said Seth Kipnis, M.D., FACS, FASMBS, director of Bariatric and Robotic Surgery at Hackensack Meridian Jersey Shore University Medical. “The new FDA guidelines for weight loss medications, including the GLP-1 drugs (which treat Type 2 diabetes and obesity), is a BMI of 30 or a BMI of 27 with at least one medical comorbidity associated with obesity.
What’s Next?
Health care providers will now see and treat any patient who meets these new FDA guidelines. “This is mainly due to the fact that GLP-1 medications are very effective at weight loss and are safe if used correctly. This change has allowed us to offer treatments for millions of more patients in the United States,” added Kipnis.
Physicians and health care providers should assess obesity-related health risks by obtaining a complete medical history, including events associated with weight gain, changes in dietary habits, genetic factors, history of exercise, current and past medications and smoking cessation. Common medications that may cause weight gain include insulin, sulphonylureas, steroids and antidepressants.
“The goal is to prevent and treat medical conditions and reverse the complications of obesity while improving quality of life,” said Asghar. “Counseling regarding further weight gain, mental health, advice on dietary habits (balanced diet, intermittent fasting) and physical activity should be incorporated.”
Under the revised guidelines, individuals with a BMI greater than 30 with one or more risk factors for cardiovascular disease who have not met weight loss goals in three to six months despite all lifestyle interventions, should receive treatment beyond counseling for diet and exercise in the form of drug therapy.
“There is a large subset of patients with comorbidities who would benefit from treatment for obesity that don’t qualify because of BMI alone. This population is at high risk and should be offered obesity management,” said Greco.
Most patients are initially offered medication; surgery is reserved for high BMI patients or those who don’t improve with medical treatments. Options depend on the severity of the disease, associated risk factors and a patient’s financial situation. Treatments range from dietary counseling, physical activity, behavioral therapy and medical treatment to more invasive treatments such as gastric sleeve, ballooning, bariatric surgery and gastric banding.
The article originally appeared in the February 6 – 12, 2025 print edition of The Two River Times.